Man Chokes Baby While Changing Diapers in Phoenix Arizona
| Choking | |
|---|---|
| Other names | Strange body airway obstruction |
 | |
| A demonstration of abdominal thrusts on a person showing signs of choking | |
| Specialty | Emergency medicine |
Choking, also known every bit foreign body airway obstruction (FBAO), is a phenomenon that occurs when breathing is impeded by a blockage inside of the throat or windpipe, resulting in oxygen impecuniousness. Although oxygen stored in the blood and lungs can keep a person alive for several minutes after breathing stops,[1] choking often leads to death.
Choking was the fourth near mutual crusade of unintentional injury-related deaths in the Usa in 2011.[2] Over four,000 choking-related deaths occur in the United states of america every yr.[three] Deaths from choking most often occur in the very young (children under 2 years old) and in the elderly (adults over 75 years).[4] [5] Foods that tin can suit their shape to that of the throat (such as bananas, marshmallows, or gelatinous candies) are more dangerous.[vi]
Providing immediate and appropriate kickoff assist can solve this blazon of choking.
Causes [edit]
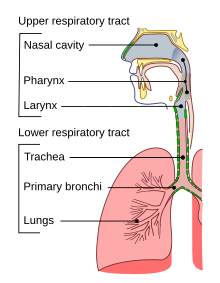
Choking happens when a foreign torso blocks the airway.[7] [8] This obstruction tin can be located in the pharynx, the larynx, or the trachea.[9] The blockage is ofttimes partial (insufficient air passes through to the lungs), just it can be complete (when the airflow is totally blocked).[9]
Foods that pose a high risk of choking include hot dogs, hard candy, nuts, seeds, whole grapes, raw carrots, apples, popcorn, peanut butter, marshmallows, chewing gum, and sausages.[7]
Amidst children, the most common causes of choking are food, coins, toys, and balloons.[7] In one study, peanuts were the most common object plant in the airway of children evaluated for suspected strange torso aspiration.[ten] In a 1984 US report, 29% of choking deaths in children were associated with latex balloons, making them the leading cause of choking deaths amongst children'due south products.[seven] Small-scale, round non-food objects such as assurance, marbles, toys, and toy parts are also associated with a high risk of choking decease because of their potential to completely block a kid's airway.[seven] Children younger than age three are especially at risk of choking because they explore their environment by putting objects in their mouths,[7] and they are however developing the ability to chew food completely.[vii] Molar teeth, which come in effectually 1.5 years of historic period, are necessary for grinding food.[seven] Even after molars are present, children go on to develop the ability to chew food completely and swallow throughout early childhood.[7] A child's airway is smaller in diameter than an adult'south airway, which means that smaller objects tin can cause airway obstacle in children. Infants and young children generate a less-forceful cough than adults, and so coughing may not be as constructive in relieving airway obstacle.[seven]
Risk factors of foreign trunk airway obstacle for people of any age include the use of alcohol or sedatives, procedures involving the oral cavity or pharynx, oral appliances, or medical conditions that crusade difficulty swallowing or impair the cough reflex;[8] conditions that can cause difficulty swallowing and/or dumb coughing include neurological conditions such as strokes, Alzheimer'south affliction, or Parkinson'southward disease.[11] In older adults, chance factors also include living solitary, wearing dentures, and having difficulty swallowing.[8] Children with neuromuscular disorders, developmental delay, traumatic brain injury, and other conditions that affect swallowing are at an increased hazard of choking.[7] Children and adults with neurological, cognitive, or psychiatric disorders may experience a delay in diagnosis because there may non be a known history of a foreign body inbound the airway.[8]
Choking on food is only one blazon of airway obstruction; others include blockage due to tumors, swelling of the airway tissues, and compression of the laryngopharynx, larynx, or vertebrate trachea in strangulation.
Prevention [edit]
Alert labels [edit]
According to a 1991 study, warning labels are an effective preventive measure against choking accidents. Items that contain many parts may include pieces that are considered choking hazards. Labels may state recommended age ranges similar on children's toys as well every bit labels alert parents to go on sure items out of the attain of children to prevent choking hazards.[12]
Master prevention [edit]
Choking ofttimes happens when large or abundant mouthfuls of food are poorly chewed and swallowed. This risk is minimized by cut food into moderately sized pieces and chewing them completely earlier swallowing.
It is helpful to have some liquid bachelor to potable to make swallowing easier. To swallow well, it is recommended that the neck be in a normal position, with the head looking frontwards and aligned with the eater's body, and that the eater be seated or continuing rather than reclining. Some activities are non very compatible with eating (such every bit laughing), so eating at the same fourth dimension increases the risk of choking. Food eaten by the handful (such as popcorn or nuts) requires chewing with more control than normal.
Unsafe foods [edit]
The foods that produce the worst cases of choking are those whose shapes adapt to the shape of the pharynx or trachea (such equally hot dogs, sausages, bananas and food in blocks).
In 2002, candy containing konjac gel was banned past the Food and Drug Assistants due to several loftier-contour choking cases.
Other foods may exist risky because they are dry in the rima oris (overcooked meat, sponge cake, common cold pizza). The chance is as well higher in tough foods (octopus, cuttlefish, reptiles or big animals), and then it is recommended cutting them into smaller chunks or thinner slices, cooking them in a way that softens them, or even eating them together with something that helps the teeth to grind them (like difficult staff of life). It is also easier to asphyxiate when eating too fast, which can usually happen in contests, games and celebrations (New Years Eve), etc.
Groups at take chances [edit]
Some population groups have a higher choking risk, such as the elderly, children, persons with disabilities (physically or mentally), people under the effects of alcohol or drugs, people who take taken medications that reduce the ability to salivate or react, patients with difficulties in swallowing (dysphagia), suicidal individuals, epileptics, and people on the autism spectrum. They may crave more than assistance to feed themselves, and it may be necessary to supervise them while they eat. People who are unable to chew properly should not be served hard food. In cases where a person is unable to safely consume, food can be given by feeding syringes. People who have taken whatever medication that reduces saliva should not eat solid nutrient until their salivation is restored.
Prevention in babies and children [edit]
All young children require care in eating, and they must acquire to chew their nutrient completely to avert choking. Feeding them while they are running, playing, laughing, etc. increases the hazard of choking. Caregivers must supervise children while eating or playing.[13] Pediatricians and dentists can provide data on various age groups to parents and caregivers nigh what nutrient and toys are appropriate to prevent choking.[seven] The American University of Pediatricians recommends waiting until half-dozen months of historic period before introducing solid foods to infants.[14] Caregivers should avoid giving children younger than 5 years one-time foods that pose a high risk of choking, such equally hot canis familiaris pieces, bananas, cheese sticks, cheese chunks, hard candy, basics, grapes, marshmallows, or popcorn.[13] Later, when they are accustomed to these foods, information technology is recommended to serve them split into small-scale pieces. Some foods as hot dogs, bananas, or grapes are usually separate lengthwise, sliced, or both. Parents, teachers, and other caregivers for children are brash to be trained in choking starting time aid and cardiopulmonary resuscitation (CPR).[7]
Children readily put small objects into their mouths (deflated balloons, marbles, minor pieces, buttons, coins, button batteries, etc.), which can lead to choking. A complicated obstacle for babies is choking on deflated balloons (including preservatives) or plastic numberless. This also includes the nappy sacks, used for wrapping the dirty diapers, which are sometimes dangerously placed near the babies.[15] To prevent children from swallowing things, precautions should be taken in the environment to go on dangerous objects out of their reach. Pocket-size children must exist supervised closely and taught to avoid putting things into their mouths. Toys and games may point on their packages the ages for which they are safe. In the United states of america, children's toy and product manufacturers are required by police to employ appropriate warning labels to their packaging,[seven] but toys that are resold may not accept them.[7] Caregivers tin try to prevent choking by considering the features of a toy (such as size, shape, consistency and small parts) before giving it to a child.[7] Children'southward products that are found to pose a choking risk can be taken off the market.[vii]
Symptoms and signs [edit]
The symptoms of choking include:
- Difficulty or disability to speak or yell.
- Inability to breathe or difficulty in animate. Labored breathing, including gasping or wheezing, may be nowadays.
- Violent and largely involuntary coughing, gurgling, or vomiting noises may be nowadays.
- Clutching of the throat (universal sign of choking). Peradventure attempting to vomit by putting fingers downwardly the throat.
- The face up turning blue (cyanosis) from lack of oxygen if breathing is not restored.
- Falling unconscious if breathing is not restored.
Times in asphyxia [edit]
The time a choking victim is still alive without brain impairment[16] tin can vary, simply typically:
- Brain damage can occur when the victim remains without air for approximately three minutes (information technology is variable).
- Death can occur if breathing is non restored in half-dozen to 10 minutes (varies depending on the victim). Still, life tin exist extended past using cardiopulmonary resuscitation for unconscious victims of choking (see more details further below).
Treatment [edit]
Choking is treated with different procedures, which form the airway management. In a general view, this consists of the anti-choking first aid techniques, in the phase of a basic airway management, and of complex methods bachelor for health professionals working in an advanced airway management.
Basic treatment (First assist) [edit]

Bones treatment of choking includes several not-invasive techniques to help remove foreign bodies from the airways.
General strategy: "V and 5" [edit]
For a conscious choking victim,[17] most institutions (equally the American Heart Clan and the American Red Cross) recommend the same full general protocol of kickoff-aid: encouraging the victim to cough, followed by hard back slaps and, if they are non constructive, applying abdominal thrusts (the Heimlich maneuver), or chest thrusts in case of the victims that can not receive pressure on the belly (encounter details farther below).
If none of those techniques are effective, the protocols recommend alternating more serial of back slaps and more series of thrusts (these on the abdomen or chest, depending of the victim), in continual turns of 5 times each one ("5 and 5").
In addition to the victims that can not receive pressure on the belly, other victims too crave specific procedures (see details further beneath), mainly the babies and the people with disabilities.
When the choking is not being solved, it is mandatory that somebody calls for emergency medical services, and standing the administration of first aid until they arrive.
If the choking victim loses consciousness,[18] [19] an anti-choking cardiopulmonary resuscitation is recommended (see more details further below).
Each one of the techniques that are part the first assistance protocol against choking are detailed below:
Coughing [edit]
If the choking individual is conscious and tin cough, the American Red Cross and the Mayo Clinic[20] recommend encouraging the individual to stay calm and go on coughing freely. It may exist easier to take air through the olfactory organ to refill the lungs.
Back blows (back slaps) [edit]

Back slaps depiction. The rescuer supports the victim's chest (for improving the effectivity) with the paw that will non slap, and bends the victim's body every bit much as possible. Then the other hand applies firm slaps.
Many associations, including the American Red Cantankerous and the Mayo Clinic,[20] [17] recommend the use of back blows (back slaps) to assistance a choking victim. This technique starts past bending the choking victim forrard as much as possible, fifty-fifty trying to place their head lower than the chest, to avoid the blows driving the object deeper into the person's throat (a rare complication, merely possible). The bending is in the back, while the cervix should non be excessively bent. It is convenient that one paw supports the victim'due south chest. Then the dorsum blows are performed by delivering forceful slaps with the heel of the hand on the victim's back, between the shoulder blades.
The back slaps push backside the blockage to expel the foreign object out. In some cases, the physical vibration of the action may cause enough move to clear the airway.
Abdominal thrusts (Heimlich maneuver) [edit]

Abdominal thrusts anti-choking technique: Employ them strongly on the expanse located between the breast and the belly button.
Abdominal thrusts[21] are performed with the rescuer standing backside the choking victim. The rescuer closes the own dominant manus, grasps it with the other paw, and presses forcefully inwards and upwards with both hands on the area located between the chest and the belly button of the victim. The pressure is non focused straight against the ribs to avoid breaking them. If the first thrust does non solve the choking, it can be repeated several times.
The use of intestinal thrusts is not recommended for infants under ane yr of age due to risk of causing injury, so there are adaptations for babies (see more details farther below), just a child that is too big for the babies' adaptations would require normal abdominal thrusts (according to the size of the body). As well, intestinal thrusts should not exist used when the victim's abdomen presents problems to receive them, such as pregnancy or excessive size; in these cases, chest thrusts are advised (see more details farther below).
In the case of choking lonely, intestinal thrusts are one of the possibilities that tin can be tried on oneself (come across more details further below).
The purpose of abdominal thrusts is to create enough pressure to expel the object lodged upward in the airway, relieving the obstruction. This method was discovered past doctor Henry Heimlich in 1974. Heimlich claimed that his maneuver was better than back blows, arguing that dorsum blows could crusade the obstruction to get more deeply lodged in the victim'due south airway. That started a fence into the medical customs,[22] that ended upwards with the recommendation of alternate both techniques, but making the patient to bend the back to foreclose complications.[23] [24] [25] In addition, the patient's chest would be supported during the back slaps.
Although it is a well known method for choking intervention, the Heimlich Maneuver is backed past limited testify and unclear guidelines. Use of the maneuver has saved many lives but can produce dire consequences if non performed correctly. This includes rib fracture, perforation of the jejunum, diaphragmatic herniation, etc.[26]
Chest thrusts [edit]

Chest thrusts anti-choking technique: If the victim cannot receive thrusts on the abdomen, employ breast thrusts. Use them strongly on the lower one-half of the chest bone, but not in the very endpoint. Avoid sticking the knuckles besides painfully into the breast.
When abdominal thrusts cannot be performed on the victim (such every bit pregnant or obese victims), breast thrusts are brash instead.[27]
Chest thrusts are performed with the rescuer standing behind the choking victim. The rescuer closes the own dominant hand and grasps it with the other hand. This tin produce several kinds of fists, but any of them can be valid if they can be placed on the victim's chest without sinking a knuckle too painfully. Keeping the fist with both hands, the rescuer uses it to printing forcefully inwards on the lower half of the chest bone (sternum). The pressure level is not focused on the very endpoint (named xiphoid process) to avoid breaking it. When the victim is a woman, the zone of the pressure level of the chest thrusts would be normally upper than the level of the breasts. If the first thrust does not solve the choking, information technology tin can be repeated several times.
Anti-choking devices [edit]
Since 2015, several anti-choking devices were developed and released to the marketplace. The design of these devices is based on a vacuum mechanical effect, with no demand for batteries or electrical electric current. They unremarkably include an fastened mask to make a vacuum from the patient'due south olfactory organ and mouth. The current models of anti-choking devices are quite similar: a direct plunger tool (LifeVac),[28] and a vacuum syringe (backward syringe) that also keeps the tongue in place by inserting a tube in the mouth (Dechoker).[29] Both of them have received certifications, and its effectiveness is proven in existent cases, some of them appeared in the media.[thirty] [31] Other mechanical models are in evolution, such as Lifewand,[32] which creates a vacuum past direct pressure against the patient'south face.
The use of approved devices can provide some advantages including: ease of usage, convenience in public places and events, being helpful for difficult cases (unconscious victims, disabled patients, elderly people, or when the victim is oneself), and achieving levels of force per unit area in suction that cannot be matched by manual methods. In the worst choking cases, no manual technique would dislodge the foreign object, being necessary the usage of one of these devices or a sort of surgery. Such concrete complications are one of the reasons why physicians recommend some care in eating. Because of the same reason, those devices are usually placed at accomplish in public and relevant places.
Withal, according to a 2020 systematic review of the effectiveness of those iii devices, "there are many weaknesses in the available data and few unbiased trials that test the effectiveness of anti-choking suction devices resulting in insufficient bear witness to support or discourage their use. Practitioners should continue to adhere to guidelines authored by local resuscitation government which marshal with ILCOR recommendations."[33]
Unconscious victims [edit]
A choking victim that becomes unconscious must be gently caught earlier falling and placed lying on a surface.[34] That surface should exist firm enough (it is recommended placing a layer of something on the floor and laying the victim above). Emergency medical services must exist called, if this has non already been washed.

Breast compressions of cardiopulmonary resuscitation (CPR).
While waiting for emergency services to arrive, the unconscious choking victim should receive a cardiopulmonary resuscitation (CPR) for choking victims, that is quite similar to the CPR for any other non-breathing patient. Infants less than one year old require a special adaptation for unconscious babies of that CPR (described farther below).
The anti-choking CPR[35] [36] for unconscious victims (being adults or children, not infants) is a wheel that alternates serial of compressions with series of ventilations (rescue breaths).

Rescue breaths of cardiopulmonary resuscitation (CPR).
Each round of compressions applies xxx compressions on the lower half of the chest bone (sternum), at an approximate rhythm of nearly 2 per second. Subsequently that serial, the rescuer looks for the obstructing object and, if it is visible, the rescuer makes a endeavour to extract it, usually by using a finger sweeping. In that location are no compressions during this step, just, if the removal complicates and takes a lot of time, it may require to repeat compressions at some moments, obviously without causing hindrances to the extraction. The object tin can exist plant and removed in this step or not, just this CPR procedure must keep anyway, until the victims tin breath by themselves or emergency medical services arrive. Next, the rescuer applies a rescue breath, pinching the victim'southward nose and puffing air inside of the mouth. Information technology is recommended, additionally, tilting the victim's caput up and downwards, to reposition it trying to open an entrance for the air, and then give an additional rescue breath. The rescue breaths would usually fail while the object is still obstructing the airway, being the well-nigh important parts the compressions and the attempts of extraction. Anyway, the rescue breaths can exist successful, and then, commonly, the chest of the victim would be seen rising. This bicycle repeats continually, starting in the 30 initial compressions.
An anti-choking device can unblock the airway on unconscious victims, but does not necessarily remove the obstructing object from the oral fissure, which may need a manual removal. The victim will then require a normal cardiopulmonary resuscitation (CPR), in the manner that has been described in a higher place but only alternate the thirty compressions and the two rescue breaths.
Most finger sweeping [edit]
In unconscious choking victims, the American Medical Association advocates sweeping the fingers across the dorsum of the throat to endeavour to dislodge airway obstructions.[37] However, many modern protocols recommend against it. Reddish Cross procedures specifically direct rescuers not to perform a finger sweep unless an object can be clearly seen in the victim's mouth to forestall driving the obstruction deeper into the victim's airway. Other protocols suggest that if the patient is conscious they will exist able to remove the foreign object themselves, or if they are unconscious, the rescuer should place them in the recovery position to allow the drainage of fluids out of the rima oris instead of downwardly the trachea due to gravity. At that place is also a risk of causing further impairment (inducing vomiting, for case) past using a finger sweep technique. In that location are no studies that have examined the usefulness of the finger sweep technique when there is no visible object in the airway. Recommendations for the use of the finger sweep accept been based on anecdotal prove.[18]
In special victims (Outset Aid) [edit]
Babies (under 1 yr erstwhile) [edit]
For babies (infants under one year old), the American Centre Clan recommends some adapted procedures.[38] Children who are too big for the babies' procedures crave the normal kickoff aid techniques against choking, co-ordinate to the size of their bodies.
First assist for babies alternates an special cycle of back blows (five dorsum slaps) followed by chest thrusts (5 adjusted chest compressions).

Back blows and breast thrusts for babies.
In the back blows maneuver, the rescuer slaps on the babe'south dorsum. It is recommended that the babe receive them being slightly leaned upside-downwards on an inclination. There exist several ways to accomplish this:
In one of the most depicted, the rescuer sits down on a seat with the baby, and supports the babe with a forearm and its respective hand. The baby's caput must exist carefully held with that hand, unremarkably by the jaw. And so the baby'southward trunk can exist leaned forward upside-down forth the rescuer's thighs and receive the slaps.
As an easier alternative, the rescuer can sit on a bed or sofa, or even the floor, carrying the infant. Next, the rescuer should support the infant'southward body on the own lap, to lean the babe upside-down at the right or the left of the lap. Then the slaps would be applied on the dorsum of the baby.
If the rescuer cannot sit down downward, at least it is possible to attempt the maneuver at a low height and over a soft surface. Then the rescuer would support the baby with a forearm and the mitt of that side, holding the baby's caput with that manus, usually by the jaw. The babe'due south body would be leaned upside-down in that position to receive the slaps.
In the chest thrusts maneuver, the baby's torso is placed lying on a surface. And so the rescuer does the compressions on the chest bone (sternum), pressing with only two fingers on its lower one-half (the nearest to the belly). Intestinal thrusts are not recommended in children less than one yr quondam because they can cause liver damage.[39]
The back blows and breast thrusts are alternated in cycles of five dorsum blows and five chest compressions until the object comes out of the baby's airway or until the infant becomes unconscious.[39]
When the choking is non being solved, it is mandatory that somebody calls to the emergency medical services. But the commencement aid has to continue until they go far.
Unconscious babies [edit]
If the infant becomes unconscious, emergency medical services must be chosen (if this has non been done still). While they come, the American Center Association[39] recommends starting an anti-choking cardiopulmonary resuscitation (CPR), which must exist adapted to babies. In that procedure, the baby is placed face-up on a firm and horizontal surface (the floor can be used). The baby's head must be in a direct position, looking frontally, because tilting also much a baby'due south head backward tin close the access to the trachea. Then, it is practical a cycle of resuscitation[twoscore] that alternates compressions and rescue breaths, similar in a normal CPR, merely with some differences:
The rescuer makes 30 compressions with only two fingers in the lower half of the chest bone (sternum), at an approximate rhythm of nearly two per second. At the finish of the round of compressions, the rescuer looks into the mouth to come across if the obstructing object has come out. And, if it is visible, the rescuer makes a try to extract information technology (mainly using a finger sweep). If the removal complicates and takes too much fourth dimension, information technology may require to repeat compressions at some moments, without hindering to the extraction. A rescuer that already knows that the choking object is a bag (or similar) does not demand to come across the object earlier trying to extract it (because there is no risk of sinking it much deeper). Being any object extracted or not, this CPR process must go along until the babies tin breath past themselves or emergency medical services make it. Next, the rescuer makes a rescue jiff, covering the babe'southward mouth and nose simultaneously with the own rima oris, and insufflating air. Despite the jammed object is an obstruction for that air blow, it must be noted that, when the airway is not clogged, just a little strenght in blowing is plenty to fill the lungs of a baby. Afterward that first rescue jiff, it is recommended tilting the babe'southward head upward and downwardly (but leaving it approximately straight once more) then requite an additional rescue breath. The probability of success of the rescue breaths is very depression while the object is withal obstructing the airway, being the nearly important parts the compressions and the attempts of extraction. Anyway, the rescue breaths tin can be successful, and and so, usually, the chest of the infant would be seen rising. This cycle repeats continually, starting in the 30 initial compressions.
Victims with issues in the belly (equally significant or obese people) [edit]
Some choking victims cannot receive pressure on their bellies, which requires changing the abdominal thrusts for chest thrusts, as the American Heart Clan recommends for them.[eighteen]
Those victims are, mainly: patients with serious injuries in the abdomen, significant women, and excessively obese people (with a size of abdomen that cannot be well managed). However, in the instance of the obese victims, if the rescuer is capable enough to manage the size of their bodies, it is possible to use the normal first aid confronting choking, with abdominal thrusts (meet details farther above).
When a proper pressure on the belly is not possible, chest thrusts are preferred. Breast thrusts are performed in a similar way to the abdominal thrusts, but with the fist placed on the lower half of the breast bone (sternum), rather than over the middle of the abdomen. As a reference, in women, the zone of pressure of the chest thrusts would be ordinarily college than the breasts. It is convenient to avoid placing the knuckles too painfully. Finally, strong inward thrusts are and then practical.[20]
The rest of the start assist protocol is the same, so the series of chest thrust are alternated with serial of slaps on the back. The back slaps are non modified: they are applied afterward bending forward the back of the victims and supporting their chest with one hand.
If choking is non being solved, somebody has to call to the emergency medical services. But it is necessary to continue trying the first aid until they arrive.
And, if the victim becomes unconscious, an anti-choking CPR for unconscious victims is needed (see details farther in a higher place).
In wheelchair, disabled victim [edit]
If the choking victim is a disabled person in a wheelchair, the procedure is quite like than in the case of the other victims. The difference is in trying to utilise the techniques directly, while the victim is seated on the wheelchair.[41] It is recommended alternate serial of back blows and thrusts, as in other cases.[42] [43]
Dorsum blows (back slaps) tin exist used after bending forrad the back of the victim very much, and supporting the victim's chest with the other mitt.
Abdominal and chest thrusts can also be used. To perform the abdominal thrusts, the rescuer must become backside the wheelchair and bend the back of the victim frontward. And so the rescuer can embrace the victim's abdomen from behind and above, leaning over the peak of the wheelchair'southward backrest. If this is too difficult, the rescuer can go down and encompass from backside the victim'southward belly and the wheelchair's backrest all together. In narrow spaces that can not be opened, the position can be accomplished past turning the victim to one side. Next, the rescuer would grasp the own hand with the other, and use them to apply sudden inward and upward pressures between the chest and the omphalos of the victim. It must be remembered that, if the victim cannot receive abdominal thrusts (in the case of pregnancy or whatsoever other problem), breast thrusts must be used instead. They are applied while the victim is in the wheelchair too, but making sudden inward pressures on the lower half of the breast os (sternum). If the space is too narrow and impossible to widen, the intestinal or chest thrusts tin be tried past turning the victim to 1 side.
When choking is not being solved, it is mandatory that somebody calls to the emergency medical services. But first aid has to go along until they arrive.
If a victim of choking in wheelchair becomes unconscious, information technology is required an anti-chocking cardiopulmonary resuscitation (CPR), that it is exactly the same one than in the case of non-disabled victims of choking. Anyway, information technology tin be noted that the victim needs to be taken from the wheelchair to be placed lying confront-up on an appropriated surface (not too hard or too soft, and it is possible to put a layer of something between the flooring and the victim). While they arrive, the rescuer has to apply the anti-choking cardiopulmonary resuscitation for unconscious victims (encounter details further in a higher place).
As a preventive measure, it is convenient to avoid placing the disabled in narrow and encased spaces at mealtimes, as more open up spaces allow easier access for rescuers. Likewise, placing an anti-choking device nearby is a common prophylactic measure out in environments with disabled people.
In bed, disabled victim [edit]
Rarely, the choking victim lays in bed, but is conscious and unable to sit down upward (such every bit in disabilities or injuries).And then the first help would be the same, but after sitting the victim on the bed'due south border.
This can be achieved[44] grasping the victim by the legs (backside of the knees, or by the calves or ankles) and rotating them until they are out of the bed. Adjacent, the rescuer would sit the victim upwardly on the edge, pulling the shoulders or artillery (in the forearms or wrists). Then it is possible to employ the anti-choking techniques[17] from behind: series of dorsum slaps (later angle very much the back of the victim, and supporting the chest with one manus) and series of abdominal thrusts (sudden compressions on the victim's belly, between the chest and the belly push). When the victim cannot receive abdominal thrusts (as in pregnancy and other cases), they must be changed for breast thrusts (sudden in pressures on the lower half of the breast os).
If a rescuer cannot sit down the victim up, it is possible to perform chest or abdominal thrusts frontally, while the victim is laying on the bed, by putting one manus on the elevation of the other and making with both of them strong pressures downwardly on the lower half of the breast bone (sternum), or in a down-and-forrard direction betwixt the breast and the belly button.
If choking is not being solved, it is mandatory that somebody calls to the emergency medical services. First assist has to go on until they arrive.
When the victims of choking in bed get unconscious, they need the same anti-choking cardiopulmonary resuscitation procedure that is employed for other unconscious choking victims (see details further above).
Preventively, it is important to know that eating while laying in bed increases the take a chance of choking. When a disabled person is present, a common mensurate of prevention is placing an anti-choking device at attain.
On the floor, disabled victim [edit]
In very rare cases, the choking victim would exist laying on the flooring merely witting, having a disability that makes impossible to sit upwards and to proceed standing up on the anxiety. And then the first help is the same, simply after sitting the victim on the floor.
So a rescuer would sit the victim up, pulling the shoulders or artillery (in the forearms or wrists). Being the victim already sitting up, the rescuer can sit behind to apply the anti-choking maneuvers, back slaps (after bending very much the back of the victim, and supporting the chest with one hand) and abdominal thrusts (sudden compressions on area that is between the chest and the umbilicus). Some victims cannot receive intestinal thrusts (as the pregnant and others), needing to modify them for breast thrusts (sudden pressures on the lower half of the breast bone).
In some situations it is impossible for a rescuer to sit the victim upward, and then the rescuer tin try one of the thrusts techniques frontally on the laying victim, putting one hand on the superlative of the other and using them to make strong pressures downwards on the lower half of the chest bone (sternum), or downwardly-and-frontwards on the abdomen (betwixt the chest and the belly button).
In case of choking is not existence solved, it is mandatory that somebody calls to the emergency medical services. Anyhow, first aid has to continue until they arrive.
In case of the victim is unconscious, it is needed the same anti-choking cardiopulmonary resuscitation process that is used in other unconscious choking victims (encounter details farther to a higher place).
In the prevention of choking, information technology can exist remembered the practice of placing an anti-choking device effectually the disabled people.
Seizing victim [edit]
Seizing tin occur for a multitude of reasons but is primarily common in those suffering from epilepsy. During a seizure, victims may experience strangulation or throat constriction during consciousness.[45] The victim will not accept control of their actual functions and will need someone to create a safe expanse for them. One should clear a space where the victim tin lay down and remove or loosen annihilation that is effectually their neck. Then one should turn them on their side equally to help them breathe and to avoid potential choking on the saliva.[46]
Self-treatment (First Aid) [edit]
Some first aid anti-choking techniques can be applied on oneself. Ane of the almost realistic options when choking solitary is having a approved anti-choking device nearby (see higher up). Simply it is also possible to try the offset assist techniques on oneself, by hand and without whatever device.
The most recommended manner consist in positioning the own abdomen over the edge of an object: mainly a chairback, simply information technology could work on an armchair, railing or countertop, and so driving the abdomen upon the edge, making sharp thrusts upwards. If the edge is not adequated, it is possible to identify a fist (even both fists) between the border and the belly, to increase the pressure level of the maneuver and make it easier (depending on the situation). It is also possible trying to fall on the edge, aiming to attain more than pressure in that way.
Likewise, abdominal thrusts tin be cocky-practical only with the easily: by making a fist, grasping it with the other paw, and pressing forcefully, inwards and upwards, with both of them on the expanse located between the breast and the omphalos, which can exist repeated many times. In the all-time of chances, it would serve equally a substitute for the abdominal thrusts of another person, despite the position in oneself is not so appropriated. Nevertheless, i study showed that these self-administered abdominal thrusts were only as effective every bit those performed by another person, although the study was made in specific weather condition and did not include obese individuals.[47]

Head-downward position for self-treatment of choking if other approaches fail.
Other variation of the self-administration of abdominal thrusts include pressing ane's own belly inwards and upwards with an appropriated object.
When a trouble makes impossible to receive pressures on the abdomen (pregnancy, too much obesity, and others), it is possible to try to utilise on oneself the breast thrusts instead of the intestinal thrusts, despite information technology would be more than hard. The chest thrusts would exist cocky-applied making a fist, grasping it with the other mitt, and pressing inwards forcefully on the lower half of the chest bone (sternum), which tin be repeated many times.
Other variation of the self-assistants of chest thrusts is the utilise of an appropriated object to press inwards in the own breast, on the lower half of the chest os (sternum).
Making attempts to cough, when it is possible, can also clear the airway.
Alternatively, multiple sources of prove suggest that one of promising approaches for self-handling during choking could be applying the head-downwardly (inverse) position.[48] [49] [18] To make that position, it is possible to put the hands on the floor and so place the knees on an upper seat (as on a bed, a sofa, or an armchair).
Advanced handling [edit]
There are many advanced medical treatments to save choking or airway obstruction, including the removal of a strange object with the assistance of a laryngoscope or bronchoscope. The use of any commercial approved anti-choking device, if it is available nearby, may exist a more than sharp solution, only brief.
A cricothyrotomy may be performed as an emergency procedure when the object cannot be removed. It involves making an incision in a patient's neck and inserting there a tube to bypass the upper airways.[50] This process is usually only performed when other methods have failed.
Epidemiology [edit]
Choking is the fourth leading cause of unintentional injury death in the Usa.[2] Many episodes go unreported considering they are brief and resolve without needing medical attention.[7] Of the reported events, 80% occur in children younger than xv years, and 20% occur in children older than 15 years.[2] Choking on a foreign object resulted in 162,000 deaths (2.5 per 100,000) in 2013, compared with 140,000 deaths (2.ix per 100,000) in 1990.[51]
Notable cases [edit]
Encounter likewise [edit]
- Pulmonary aspiration
- Basic airway direction
- BLS
- Breathing
- Oxygen Deprivation
- Cognitive Hypoxia
References [edit]
- ^ Ross, Darrell Lee; Chan, Theodore C (2006). Sudden Deaths in Custody. ISBN978-1-59745-015-seven.
- ^ a b c "Injury Facts 2015 Edition" (PDF). National Safety Council. Archived from the original (PDF) on 26 September 2017. Retrieved 1 Dec 2017.
- ^ Chillag, Shawn; Krieg, Jake; Bhargava, Ranjana (2010-02-01). "The Heimlich Maneuver: Breaking Downwards the Complications". Southern Medical Journal. 103 (2): 147–150. doi:10.1097/SMJ.0b013e3181c99140. ISSN 0038-4348. PMID 20065901. S2CID 19387827.
- ^ National Safety Council. Inquiry and Statistics Department. (2015). Injury facts (2015 ed.). Itasca, IL. ISBN9780879123345. OCLC 910514461.
- ^ Pavitt, Matthew J.; et al. (2017). "Choking on a strange trunk: a physiological report of the effectiveness of abdominal thrust maneuvers to increment thoracic pressure". Thorax. 72 (6): 576–78. doi:10.1136/thoraxjnl-2016-209540. PMC5520267. PMID 28404809.
- ^ Sayadi, Roya (May 2010). Swallow Safely: How Swallowing Problems Threaten the Elderly and Others (First ed.). Natick, MA: Inside/Outside Press. pp. 46–47. ISBN9780981960128.
- ^ a b c d e f chiliad h i j k l m northward o p q r Committee on Injury, Violence (2010-03-01). "Prevention of Choking Among Children". Pediatrics. 125 (iii): 601–607. doi:ten.1542/peds.2009-2862. ISSN 0031-4005. PMID 20176668.
- ^ a b c d Warshawsky, Martin (31 December 2015). "Foreign Body Aspiration". Medscape . Retrieved 1 December 2017.
- ^ a b Dominic Lucia; Jared Glenn (2008). Current Diagnosis & Handling: Emergency Medicine. New York: McGraw-Hill. ISBN978-0-07-184061-3.
- ^ Yadav, S. P.; Singh, J.; Aggarwal, Northward.; Goel, A. (September 2007). "Airway foreign bodies in children: experience of 132 cases". Singapore Medical Journal. 48 (9): 850–853. ISSN 0037-5675. PMID 17728968.
- ^ Boyd, Michael; Chatterjee, Arjun; Chiles, Caroline; Chin, Robert (2009). "Tracheobronchial Foreign Body Aspiration in Adults". Southern Medical Periodical. 102 (2): 171–174. doi:10.1097/smj.0b013e318193c9c8. PMID 19139679. S2CID 5401129.
- ^ Langlois, Jean A. (1991-06-05). "The Bear upon of Specific Toy Warning Labels". JAMA: The Periodical of the American Medical Clan. 265 (21): 2848–2850. doi:10.1001/jama.1991.03460210094036. ISSN 0098-7484. PMID 2033742.
- ^ a b "Choking Prevention for Babies". Rubber Kids Worldwide . Retrieved 2017-12-15 .
- ^ "Infant Food and Feeding". world wide web.aap.org . Retrieved 2017-12-15 .
- ^ "Campaign Confronting Nappy Sacks". Imperial Lodge for the Prevention of Accidents.
- ^ "How Long Can the Brain Be without Oxygen earlier Brain Damage?". 2021-04-06. Archived from the original on 2021-04-06. Retrieved 2021-05-22 .
- ^ a b c "Witting Choking" (PDF). American Cerise Cantankerous. Archived (PDF) from the original on 2020-01-31.
- ^ a b c d "Part 5: Adult Basic Life Support and Cardiopulmonary Resuscitation Quality – ECC Guidelines". eccguidelines.center.org . Retrieved iv December 2017.
- ^ "STEP 3: Be Informed – Witting Choking | Exist Cherry-red Cross Ready". redcross.org . Retrieved 4 December 2017.
- ^ a b c Mayo Clinic. "Choking: Offset assist". Mayo Foundation for Medical Education and Research (MFMER). Archived from the original on 7 January 2019. Retrieved 4 December 2017.
- ^ "First Aid Tips". Red Cantankerous. Archived from the original on 2009-02-03.
- ^ Mills Senn, Pamela (April 2007). Cincinnati Magazine. Emmis Communications. p. 92.
- ^ American Cherry-red Cross. "New First Aid and CPR/AED Training Programs". Archived from the original on 2006-04-29. Retrieved 2021-11-07 .
- ^ "Choking: First aid". Mayo Clinic . Retrieved 2021-11-07 .
- ^ "Conscious Choking" (PDF). Archived (PDF) from the original on 2020-01-31. Retrieved 2021-11-07 .
- ^ Fearing, Nicole G.; Harrison, Paul B. (2002-11-02). "Complications of the Heimlich Maneuver: Case Report and Literature Review". The Periodical of Trauma: Injury, Infection, and Critical Care. 53 (5): 978–979. doi:10.1097/00005373-200211000-00026. ISSN 0022-5282. PMID 12435952.
- ^ "Choking and CPR safety talk". Oklahoma State University. Archived from the original on 2020-01-30.
- ^ "How to use LifeVac". Lifevac.life. 2016-08-02. Retrieved 2020-01-20 .
- ^ Dechoker. "How to Use Dechoker Anti-Choking Device (ACD)". Dechoker . Retrieved 2020-01-20 .
- ^ "Advocates say anti-choking device saved 2 lives in Idaho | Local | idahostatejournal.com". 2019-02-03. Archived from the original on 2019-02-03. Retrieved 2021-09-25 .
- ^ "Carers used suction device to save woman who choked on sausage". Kidderminster Shuttle . Retrieved 2021-09-25 .
- ^ "lifewand - keep kids safe". lifewand.com . Retrieved 2020-01-20 .
- ^ Dunne, Cody (2020). "A systematic review on the effectiveness of anti-choking suction devices and identification of research gaps". Resuscitation. 153: 219–226. doi:10.1016/j.resuscitation.2020.02.021. PMID 32114068. S2CID 211725361.
- ^ H R H (2021-x-26). "The American Medical Association??s Handbook of First Help and Emergency Care". Journal of Occupational and Environmental Medicine. 23 (2): 74. doi:ten.1097/00043764-198102000-00004. ISSN 1076-2752.
- ^ American Red Cross. "Unconscious Choking". CPR/AED and First Aid. p. 22.
- ^ "Instructor's Corner". americanredcross.force.com . Retrieved 2020-01-xix .
- ^ American Medical Association (2009-05-05). American Medical Association Handbook of Offset Aid and Emergency Care . Random House. ISBN978-1-4000-0712-seven.
dislodge the object.
- ^ Wilkins, Lippincott Williams (2010-11-02). "Editorial Board". Apportionment. 122 (18_suppl_3): S639. doi:10.1161/CIR.0b013e3181fdf7aa.
- ^ a b c Wilkins, Lippincott Williams & (2010-11-02). "Editorial Board". Circulation. 122 (18 suppl three): S639. doi:10.1161/CIR.0b013e3181fdf7aa. ISSN 0009-7322.
- ^ American Crimson Cross. "Choking - Special Situations". CPR/AED and Start Aid. p. 33.
- ^ "Choking Awareness, wheelchair user" (PDF). Belfast Health and Social Care Trust.
- ^ "Conscious Choking" (PDF). American Cerise Cross. Archived (PDF) from the original on 2020-01-31.
- ^ "Choking Awareness, wheelchair user" (PDF). Belfast Health and Social Care Trust.
- ^ "Profitable a Patient to a Sitting Position and Ambulation". Medicine LibreTexts. 2018-12-22. Archived from the original on 2021-10-07. Retrieved 2021-xi-07 .
- ^ Nimeshan, Geevasinga (2000-12-08). "Choking, Asphyxiation, and the Insular Seizure". Journal of Clinical Neuroscience: i–sixteen. doi:10.1054/jocn.1999.0776. ISSN 0967-5868.
- ^ "Seizure Start Help | Epilepsy | CDC". www.cdc.gov. 2020-09-xxx. Retrieved 2021-12-08 .
- ^ Pavitt MJ, Swanton LL, Hind Thou, et al. (12 Apr 2017). "Choking on a foreign torso: a physiological study of the effectiveness of intestinal thrust manoeuvres to increase thoracic pressure". Thorax. 72 (6): 576–578. doi:10.1136/thoraxjnl-2016-209540. PMC5520267. PMID 28404809.
- ^ Luczak, Artur (2019). "Effect of body position on relieve of foreign body from the airway†". AIMS Public Health. 6 (ii): 154–159. doi:10.3934/publichealth.2019.2.154. ISSN 2327-8994. PMC6606524. PMID 31297401.
- ^ Luczak, Artur (June 2016). "Head-down cocky-handling of choking". Resuscitation. 103: e13. doi:10.1016/j.resuscitation.2016.02.015. ISSN 0300-9572. PMID 26923159.
- ^ "What is a trachceostomy?". Retrieved 25 February 2014.
- ^ GBD 2013 Bloodshed and Causes of Death, Collaborators (17 December 2014). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of expiry, 1990–2013: a systematic assay for the Global Burden of Affliction Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(xiv)61682-2. PMC4340604. PMID 25530442.
External links [edit]
- Choking at Curlie
carrollsaineve1990.blogspot.com
Source: https://en.wikipedia.org/wiki/Choking
0 Response to "Man Chokes Baby While Changing Diapers in Phoenix Arizona"
Postar um comentário